

Time:2026-04-30 Form:本站
Implant Torque and Stability Explained: What Distributors Should Know Before Choosing an Implant System
In dental implantology, “torque” and “stability” are often mentioned together, but they are not the same thing. For dentists, these concepts affect surgical confidence, loading decisions, and long-term treatment predictability. For distributors and implant buyers, they affect something equally important: whether an implant system performs consistently in real clinical use.
A dental implant may look simple from the outside—a threaded titanium fixture placed into bone—but its performance depends on a combination of design, surface, connection accuracy, drilling protocol, bone quality, and surgical handling. Among these factors, insertion torque and primary stability are two of the most discussed indicators during placement.
However, a common misunderstanding exists in the market: higher torque does not always mean better implant stability. In some cases, excessive torque may increase compression on bone and create biological risk. In other cases, insufficient torque may make immediate loading unsafe or reduce clinician confidence.
This article explains implant torque and stability in a practical, B2B-focused way. It is written for dental implant distributors, procurement teams, OEM buyers, and professionals evaluating implant systems for their markets.
Implant torque usually refers to insertion torque, the rotational force required to place a dental implant into prepared bone. It is commonly measured in Ncm, or Newton-centimeters.
During implant placement, the implant is rotated into the osteotomy site. The resistance felt during this insertion is recorded as torque. In simple terms, insertion torque reflects how tightly the implant engages with the surrounding bone at the time of placement.
For example:
Insertion Torque Range | General Meaning |
Low torque | Weak bone engagement or oversized osteotomy |
Moderate torque | Controlled primary fixation |
High torque | Strong mechanical engagement, but possible bone compression |
Excessive torque | Potential risk of over-compression or implant/component stress |
Clinically, insertion torque is one of the first pieces of feedback a dentist receives during implant placement. It tells the clinician whether the implant feels secure enough for healing, provisionalization, or possible immediate loading.
But torque alone does not tell the full story.
Implant stability refers to the implant’s resistance to movement after placement. It can be divided into two major types:
Primary stability is the mechanical stability achieved immediately after the implant is inserted. It depends mainly on:
l Bone density
l Implant macro-design
l Thread geometry
l Implant diameter and length
l Osteotomy preparation
l Surgical technique
l Insertion torque
l Bone-to-implant contact at placement
Primary stability is especially important in immediate placement and immediate loading cases.
Secondary stability is the biological stability that develops during healing. It comes from osseointegration, where bone grows and remodels around the implant surface.
Secondary stability depends more on:
l Implant surface treatment
l Biocompatibility of titanium material
l Healing time
l Bone metabolism
l Surgical trauma control
l Absence of micromovement
l Prosthetic loading management
A good implant system must support both types of stability. Strong initial fixation is useful, but long-term success depends on biological integration.
No. Implant torque and implant stability are related, but they are not identical.
Insertion torque measures rotational resistance during placement. Stability measures resistance to micromovement after placement.
An implant can have high insertion torque but not necessarily ideal biological stability. For example, if an implant is forced into dense cortical bone with excessive pressure, torque may be high, but bone compression may negatively affect healing.
On the other hand, an implant placed with moderate torque may still achieve excellent stability if the thread design, osteotomy protocol, and bone conditions are appropriate.
A better way to understand it:
Factor | Torque | Stability |
What it measures | Rotational resistance during insertion | Resistance to movement after placement |
Main timing | During surgery | During and after healing |
Main nature | Mechanical | Mechanical + biological |
Measurement unit | Ncm | ISQ, clinical assessment, mobility testing |
Higher is always better? | No | Generally yes, if biologically healthy |
Influenced by implant design? | Yes | Yes |
Influenced by surface treatment? | Limited during insertion | Strongly during healing |
For implant distributors, this distinction matters because some manufacturers may promote high insertion torque as if it automatically proves superior implant quality. In reality, the implant should offer controlled insertion behavior, stable engagement, and predictable osseointegration—not simply aggressive cutting into bone.
Insertion torque matters because it gives immediate information about how the implant is engaging the bone. It helps dentists decide whether the implant can be restored immediately, covered for healing, or monitored more cautiously.
If the implant reaches a reasonable insertion torque, the clinician may feel confident that the implant has achieved mechanical engagement.
This is especially important in:
l Soft bone cases
l Posterior maxilla cases
l Immediate extraction socket placement
l Short implant placement
l Immediate provisionalization
l Full-arch treatment
l Guided surgery cases
Immediate loading usually requires good primary stability. Many clinicians use insertion torque as one factor when deciding whether to attach a temporary crown, bridge, or full-arch prosthesis soon after surgery.
However, torque should not be the only criterion. ISQ value, bone quality, implant distribution, occlusion, and prosthetic design also matter.
A well-designed implant system should have a matching surgical kit and drilling sequence. If the drill protocol is too aggressive, torque may be low. If the osteotomy is too narrow, torque may become excessive.
That is why implant systems should not be judged only by fixture shape. The full system—implant, drills, taps, drivers, and protocol—must work together.
Many buyers assume higher torque means better quality. This is not always true.
Excessive insertion torque may create several risks:
Too much torque may compress cortical bone excessively. Bone is living tissue, not just a mechanical material. Over-compression may reduce blood supply and affect healing.
If torque rises because the osteotomy is too tight, insertion may generate more friction. Combined with poor irrigation or dense bone, this can increase surgical trauma.
Very high torque can also place stress on the implant body, internal connection, mount, or driver. For distributors, this matters because component damage can create complaints even when the fixture itself is made from good titanium.
A high insertion torque number may make the dentist feel safe, but if the implant is overloaded too early or if the bone is damaged by compression, long-term stability may still be compromised.
The goal is not maximum torque. The goal is controlled, appropriate torque for the case.
There is no single universal “best” torque value for every implant case. Different clinical situations require different decisions.
In general, many clinicians consider moderate-to-high insertion torque helpful for immediate loading, while lower torque may require submerged healing or delayed loading.
A practical view:
Torque Level | Clinical Interpretation |
Below 20 Ncm | May indicate limited primary stability |
20–35 Ncm | Often acceptable for conventional healing |
35–45 Ncm | Commonly considered favorable for many loading decisions |
Above 45–50 Ncm | Strong engagement, but should be evaluated carefully |
Very high torque | May suggest excessive compression depending on bone and protocol |
For B2B buyers, the key point is not to market one number as perfect. Instead, a reliable implant system should provide predictable torque behavior across different bone types when used with the correct protocol.
ISQ means Implant Stability Quotient. It is usually measured using resonance frequency analysis. ISQ gives a numerical value that reflects implant stability after placement.
The ISQ scale usually ranges from 1 to 100. Higher ISQ generally indicates greater stability.
Measurement | What It Shows |
Insertion torque | Resistance during implant placement |
ISQ | Stability after implant placement |
Periotest or mobility test | Resistance to movement |
Clinical judgment | Overall case-based decision |
Torque is measured during insertion. ISQ can be measured immediately after placement and again during healing. This makes ISQ useful for monitoring stability changes over time.
A typical healing curve may show that primary stability decreases slightly as bone remodels, while secondary stability increases as osseointegration develops. A good implant system should support a smooth transition from mechanical stability to biological stability.
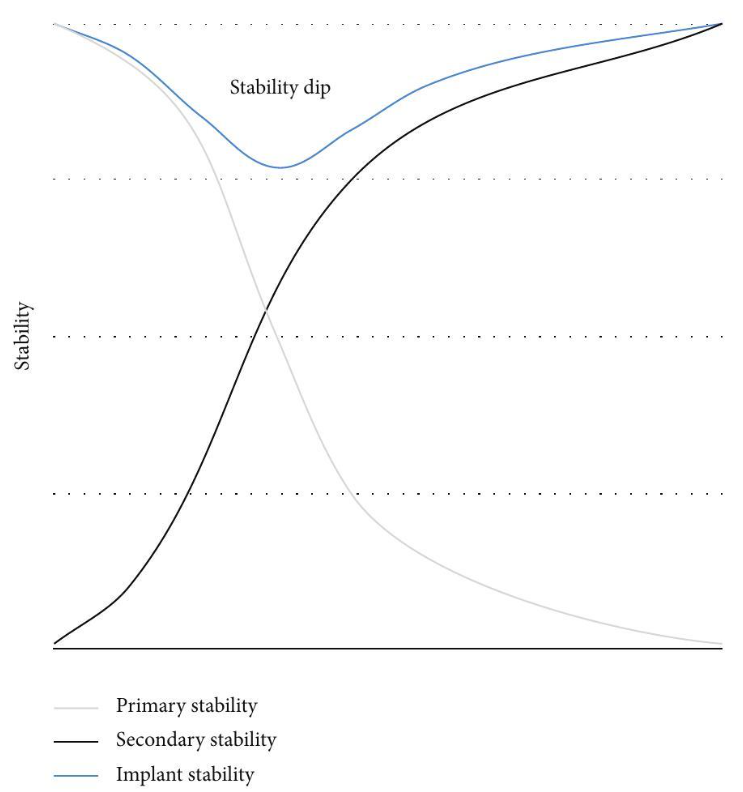
One of the most important concepts in implant stability is the “stability dip.” After implant placement, mechanical stability may decrease temporarily as bone remodeling begins. At the same time, biological stability has not yet fully developed.
This transition period is critical.
If the implant experiences excessive micromovement during this phase, osseointegration may be affected. That is why loading protocol, occlusal control, prosthetic design, and patient behavior are important.
For distributors, this is important because implant success is not only about the fixture. Dentists need a system that includes:
l Clear drilling protocols
l Reliable prosthetic components
l Accurate connections
l Stable abutment fit
l Compatible restorative options
l Consistent surface treatment
l Practical clinical instructions
A factory that only focuses on producing the fixture body but ignores the full system may struggle to deliver consistent market performance.
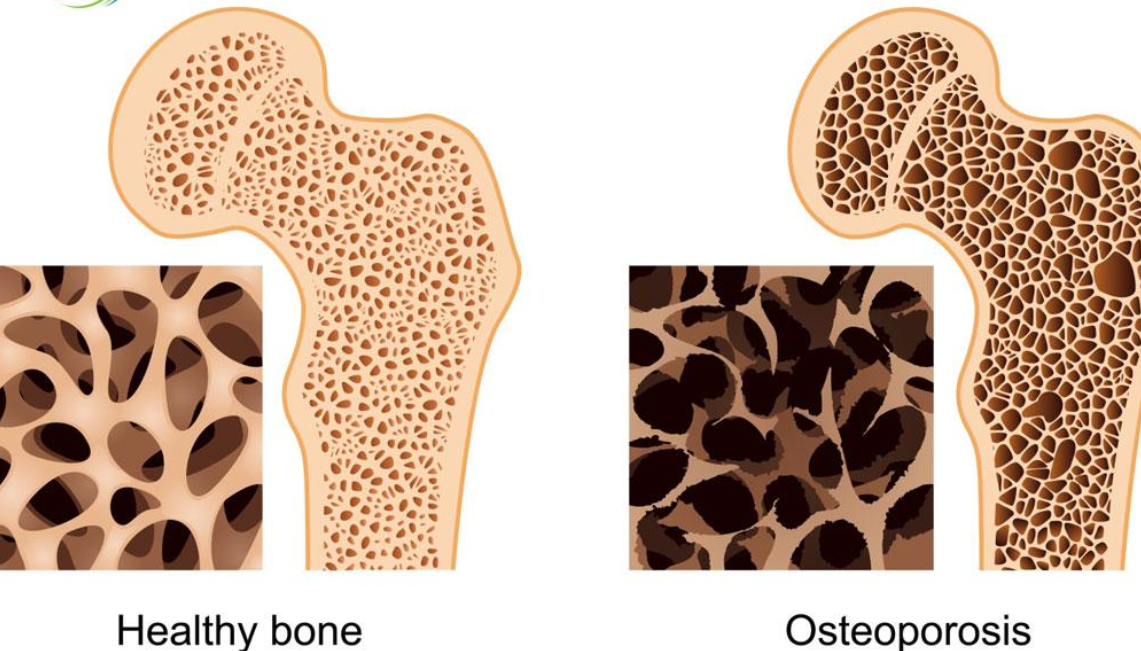
Bone quality has a major influence on both insertion torque and implant stability.
Dense cortical bone often produces higher insertion torque. However, dense bone also requires careful drilling, tapping, and heat control.
If the osteotomy is underprepared too much, torque may rise sharply. This may feel secure but can create compression risk.
Soft bone usually produces lower torque. This is common in the posterior maxilla. In soft bone, implant design becomes especially important.
Features that may help include:
l Tapered implant body
l Deeper threads
l Condensing thread design
l Self-tapping ability
l Optimized drilling sequence
l Wider implant selection
l Longer healing period when needed
A strong implant system should offer different options for different bone conditions instead of relying on one universal design for every case.
Implant macro-design plays a direct role in insertion behavior and primary stability.
Tapered implants often provide stronger engagement in soft bone and extraction sockets. They can help improve primary stability, but if used aggressively in dense bone, they may increase compression.
Deeper threads may improve engagement in soft bone. However, thread geometry must be balanced to avoid excessive insertion resistance.
Thread pitch affects how quickly the implant advances during insertion and how force is distributed to surrounding bone.
Self-tapping grooves help the implant cut into bone during placement. This can reduce insertion difficulty and improve control.
The apex affects insertion guidance, socket engagement, and safety near anatomical structures. A sharp aggressive apex may improve initial bite but must be designed carefully.
Internal connection accuracy does not directly create insertion torque, but it affects long-term prosthetic stability. Poor connection fit may lead to screw loosening, microgap problems, or restorative complaints.
This is where manufacturing quality becomes important. For example, RE-TECH focuses on implant systems and compatible prosthetic components where fixture design, connection tolerance, and restorative workflow need to work as one system rather than as isolated parts.
Surface treatment does not usually create insertion torque, but it strongly affects secondary stability.
Modern implant surfaces are designed to support bone response by increasing surface area, improving wettability, or creating micro-roughness.
Common surface concepts include:
l SLA-type roughened surfaces
l Sandblasted and acid-etched surfaces
l Hydrophilic surfaces
l RBM-treated surfaces
l Anodized surfaces
The purpose is not simply to make the implant look rough. The goal is to create a controlled surface that supports bone attachment and biological integration.
For buyers, surface consistency is extremely important. Two implants may claim the same surface type, but actual performance depends on process control, cleaning, contamination management, packaging, and inspection.
Even the best implant design can perform poorly if the drilling protocol is wrong.
The osteotomy determines how the implant interacts with bone. If the site is too wide, torque may be low. If it is too narrow, torque may be excessive.
Important protocol factors include:
l Final drill diameter
l Drill depth
l Drill speed
l Irrigation
l Bone density classification
l Use of countersink
l Use of bone tap
l Guided vs freehand surgery
l Implant diameter selection
For distributors, this means the implant supplier should provide more than a product catalog. They should provide clear surgical guidance, drilling charts, and training support.
A complete system is easier for dentists to trust and easier for distributors to promote.
Immediate loading is one of the areas where torque and stability are most often discussed.
Immediate loading means attaching a temporary or definitive prosthesis soon after implant placement. This can be attractive for patients and clinics, but it requires careful case selection.
Factors that influence immediate loading decisions include:
l Insertion torque
l ISQ value
l Bone quality
l Number of implants
l Implant distribution
l Prosthetic splinting
l Occlusal forces
l Patient habits
l Implant length and diameter
l Surgical accuracy
High torque alone does not guarantee immediate loading success. The implant must resist micromovement during healing.
For full-arch cases, splinting multiple implants can improve stability. For single implants, immediate loading may be more sensitive to occlusion and primary fixation.
Implant failure is rarely caused by one single factor. However, poor torque control and insufficient stability can contribute to complications.
Possible risk situations include:
If the implant lacks primary fixation, micromovement may occur during healing.
Over-compression may affect bone vitality and healing response.
An unsuitable osteotomy can create either low torque or excessive torque.
A design that does not match real clinical needs may perform inconsistently across bone types.
Even if the implant integrates well, poor abutment fit or screw instability can cause long-term issues.
Contamination or inconsistent surface treatment may affect osseointegration.
This is why distributors should evaluate implant systems from a full-system perspective, not only by price or fixture appearance.
Before choosing an implant supplier, distributors should ask technical questions related to torque and stability.
l Is the implant tapered, parallel-walled, or hybrid?
l What bone types is the implant design best suited for?
l How does the thread design improve primary stability?
l Is the implant self-tapping?
l What torque range is recommended?
l What is the maximum recommended insertion torque?
l Are there different drilling protocols for soft and dense bone?
l Is a countersink recommended?
l Is tapping required in dense bone?
l Are guided surgery drills available?
l Is the protocol simple enough for daily clinical use?
l What surface treatment is used?
l How is surface cleanliness controlled?
l What inspection process is used?
l Are implants packaged in a controlled environment?
l Are batch records and traceability available?
l Are healing abutments, impression copings, scan bodies, and Ti-bases available?
l Is the connection compatible with common restorative workflows?
l Are prosthetic screws stable and consistent?
l Are digital libraries available?
A reliable implant supplier should be able to answer these questions clearly. If answers are vague, distributors should be careful.
For implant distributors, the product must do more than pass a basic specification. It must perform consistently in the hands of many clinicians.
A distributor may lose market trust if dentists report:
l Unstable insertion feel
l Driver stripping
l Inconsistent torque
l Complicated drilling protocol
l Screw loosening
l Poor prosthetic compatibility
l Unclear instructions
l Lack of component availability
On the other hand, a stable implant system can help distributors build repeat orders and clinician loyalty.
This is where manufacturers like RE-TECH can be naturally evaluated: not only as a fixture producer, but as a system supplier offering implant bodies, prosthetic components, and compatibility-oriented solutions for distributor markets. For B2B buyers, that full-system thinking is often more valuable than simply choosing the lowest fixture price.
Not true. Higher torque may reflect strong engagement, but it can also indicate excessive compression.
Not true. ISQ, bone quality, prosthetic design, and occlusion also matter.
Not necessarily. With the right implant design and drilling protocol, soft bone can be managed successfully.
Surface treatment mainly supports biological healing, not insertion resistance.
No. Compatibility requires precise connection geometry, consistent tolerance, and reliable prosthetic components.
Feature | High-Torque-Focused System | Balanced-Stability System |
Main selling point | Strong insertion resistance | Controlled mechanical and biological performance |
Risk | Over-compression in dense bone | Requires proper protocol selection |
Best use | Selected soft bone cases | Wider clinical indications |
Distributor advantage | Easy marketing message | Better long-term clinician trust |
Clinical flexibility | May be limited | Usually stronger |
Key requirement | Careful torque control | Good design + protocol + surface |
For long-term distribution, a balanced-stability system is usually easier to build around. Dentists do not only want an implant that feels tight. They want an implant that heals predictably, restores smoothly, and creates fewer complications.
Many manufacturers claim “excellent primary stability.” Buyers should ask for details.
A good supplier should explain:
l What design feature improves stability
l Which bone types the implant is designed for
l What torque range is recommended
l How the drilling protocol changes by bone density
l Whether clinical or mechanical testing data is available
l How surface consistency is controlled
l How connection tolerance is inspected
Avoid suppliers that only use general language like “high quality,” “premium design,” or “strong stability” without technical support.
For distributors, the best supplier is not always the one with the most aggressive marketing. It is the one that can help you explain the system clearly to dentists.
Insertion torque is the rotational force required to place a dental implant into bone. It is usually measured in Ncm and reflects mechanical engagement during placement.
No. Very high torque may create excessive bone compression. The ideal torque depends on bone quality, implant design, drilling protocol, and loading plan.
Primary stability is the mechanical fixation of the implant immediately after placement. It depends on bone density, implant design, osteotomy preparation, and insertion technique.
Secondary stability is biological stability that develops through osseointegration. It depends on healing, implant surface, bone response, and loading control.
ISQ stands for Implant Stability Quotient. It is a numerical value used to assess implant stability, often through resonance frequency analysis.
Yes. High torque does not always guarantee ideal stability. If high torque comes from excessive bone compression or poor protocol, healing may still be at risk.
There is no universal number for all cases. Many clinicians prefer stronger insertion torque and good ISQ values before immediate loading, but the decision must also consider bone quality, occlusion, and prosthetic design.
Implant body shape, thread depth, thread pitch, self-tapping design, apex shape, and diameter all affect primary stability and insertion behavior.
Surface treatment mainly affects secondary stability by supporting osseointegration. It does not replace the need for good primary mechanical fixation.
Distributors should check implant design, drilling protocol, torque recommendations, surface treatment, prosthetic compatibility, packaging, traceability, and technical support.
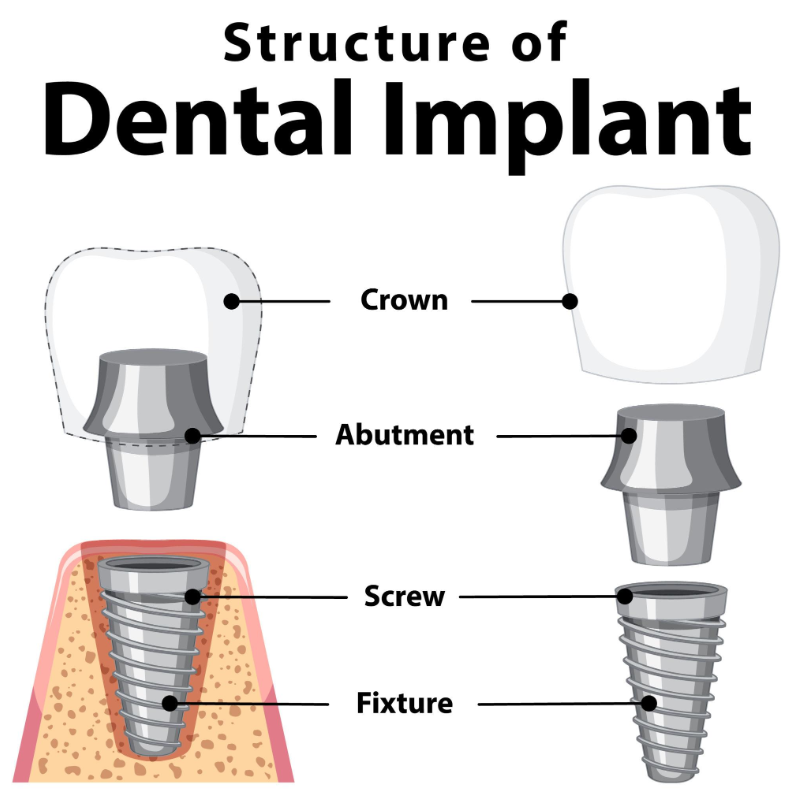
Implant torque and stability are closely related, but they are not the same. Torque shows how the implant engages bone during insertion. Stability reflects how well the implant resists movement during healing and function.
For clinicians, this affects surgical decisions and loading protocols. For distributors, it affects product reputation, repeat orders, and market trust.
A strong implant system should not simply chase high torque numbers. It should provide controlled insertion, reliable primary stability, consistent surface quality, accurate prosthetic fit, and clear surgical protocols.
For B2B buyers evaluating implant systems, the best question is not “Which implant has the highest torque?” The better question is: “Which implant system gives dentists predictable stability across different clinical conditions?”
That is the kind of answer that builds long-term confidence in the market.
Prev:Import and Shipping Dental Implants: A Practical Guide for Distributors
Next:No More